Musculoskeletal Disorders: Fracture
The iSavta Team | 13.11.2019
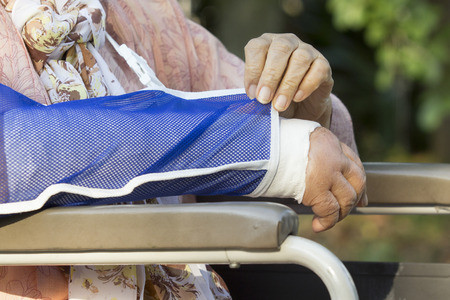
A fracture is a broken bone. A closed fracture (simple fracture) means the bone is broken but the skin is intact. In an open fracture (compound fracture), the broken bone has come through the skin.
Falls, accidents, cancer and osteoporosis are causes. Signs and symptoms include pain, swelling, limited movements, loss of function, bruising and bleeding.
For healing, the bone ends are brought into normal position. This is called reduction. Closed reduction involves moving the bone back into place. The skin is not opened. Open reduction involves surgery. The bone is exposed and brought back for alignment. Nails, rods, pins, screws, plates, or wires keep the bone in place. After reduction, bone movement is prevented with cast or traction.
Casts are made of plaster of Paris, plastic, or fiber-glass. Plastic and fiberglass casts dry quickly. A plaster of Paris cast needs 24 to 48 hours to dry. It is odorless, cool and has a musty smell.
With traction, a steady pull from two directions keeps the fractured bone in place. Ropes, pulleys, and weights are used. Traction is applied to the neck, arms, legs, or pelvis.
Rules for Cast Care
- Do not cover the cast with blankets, plastic, or other material. A plaster cast gives off heat as it dries. Covers prevent the escape of heat. If heat cannot escape, burns can occur.
- Turn the person as directed to promote even drying of cast.
- Do not place a wet cast on a hard surface. It flattens the cast. The cast must keep its shape. Use pillows to support the entire length of the cast.
- Support a wet cast with your palms when turning and positioning the person. Fingers can dent the cast. Dents can cause pressure areas that can lead to skin breakdown.
- Report rough cast edges. The nurse will need to cover the cast edges with tape.
- Keep a plaster cast dry. A wet plaster cast loses its shape. After the cast dries, the nurse may apply a waterproof material around the perineal area to protect the cast from moisture.
- Do not let the person insert things into the cast. Itching under the cast causes an intense desire to scratch. Items used for scratching (pencils, coot hangers, knitting needles, back scractchers) can open the skin. An infection can develop. Scratching item can wrinkle the stockinette or be lost into the cast. Both can cause pressure and lead to skin breakdown.
- Elevate a casted arm or leg on pillows. This reduces swelling.
- Have enough help when turning and repositioning the person. Plaster casts are heave and awkward. Balance is lost easily.
- Position the person as the nurse and care plan direct.
- Report these signs and symptoms immediately:
- Pain – pressure ulcer, poor circulation, or nerve damage.
- Swelling and a tight cast – reduced blood flow to the part.
- Pale skin - reduced blood flow to the part.
- Cyanosis - reduced blood flow to the part.
- Odor – infection.
- Inability to move the fingers or toes – pressure on a nerve.
- Numbness - pressure on a nerve or reduced blood flow to the part.
- Temperature changes – cool skin means poor circulation; hot skin means inflammation.
- Drainage on or under the cast – infection.
- Chills, fever, nausea, and vomiting – infection.
Caring for Persons in Traction
- Keep the person in good alignment.
- Do not remove the traction.
- Keep weights off the floor. They must hang freely from the traction setup.
- Do not add or remove weights from the traction setup.
- Perform range-of-motion exercises for the uninvolved body parts as the nurse directs.
- Position the person as the nurse directs. Usually only the back-lying position is allowed. Sometimes slight turning is allowed.
- Provide the fracture pan for elimination.
- Give skin care. Follow the care plan.
- Put bottom linens on the bed from the top down. The person uses the trapeze to raise the body off the bed.
- Check pin, nail, wire, or tong sites for redness, drainage, or odors. Report observations to the nurse immediately.
- Observe for signs and symptoms in Rules for Cast Care. Report any to the nurse immediately.
Hip Fractures
Fractured hips are common in older persons. They are very serious because healing is slower in older people. Open reduction is usually required. The fracture is fixed in position with a pin, nail, plate, screw, or prosthesis. Rehabilitation is needed after surgery. Postoperative complications are great risks. They include pneumonia, urinary tract infection, and thrombi in the leg veins. The person can die from these complications. Pressure ulcers and confusion are other risks.
Care of the Person with a Hip Fracture
- Give good skin care. Skin breakdown occurs rapidly.
- Encourage coughing and breathing exercises as directed.
- Turn and reposition the person as directed. Usually the person is not positioned on the operative side.
- Keep the operated leg abducted at all times. It is abducted when the person is supine, being turned, or in a side-lying position. Use pillow or abductor splints as directed.
- Prevent external rotation (turning outward) of the hip. Use trochanter rolls, pillows, sandbags, or abduction splints as directed.
- Perform range-of-motion exercises as directed. Do not exercise the affected leg.
- Provide a straight-back chair with armrests. The person needs a high, firm seat. A low, soft chair is not used.
- Place the chair on the unaffected side.
- Assist the nurse in transferring the person.
- Do not let the person stand on the operated leg unless allowed by the doctor.
- Support and elevate the leg as directed when the person is sitting on the chair.
- Apply elastic stockings as directed.
- Remind the person not to cross the legs when seated.












